Strategies for Cure: Stem Cell Lymphocytic Leukemia Treatment and Procedures
Lymphocytic leukemia, whether it presents as the acute, rapid-onset form (ALL) or the chronic, slower-developing form (CLL), poses a significant challenge to the body’s immune system. While the diagnosis can be daunting, advancements in medical science have transformed the landscape of recovery. Today, a combination of targeted drug therapies and advanced stem cell procedures offers many patients a realistic path to long-term remission and cure.
Understanding the hierarchy of treatment from initial chemotherapy to the complexities of transplantation—is essential for patients and families navigating this journey.
The Treatment Landscape: Induction and Consolidation
The primary goal of leukemia treatment is to achieve remission, a state where no cancer cells are detectable in the body.
- Induction Therapy: This is the first phase, typically involving intensive chemotherapy or corticosteroids to kill as many leukemia cells as possible and restore normal blood production.
- Targeted Therapy: Especially in Chronic Lymphocytic Leukemia (CLL), modern drugs can target specific proteins within cancer cells to stop them from growing, often sparing healthy cells more effectively than traditional chemo.
However, for high-risk patients or those whose leukemia returns (relapse), standard therapies may not be enough. This is where the specific Stem Cell Lymphocytic Leukemia Treatment and Procedures become the critical next step in the curative process.
The Role of Stem Cell Transplantation
A stem cell transplant (often called a bone marrow transplant) is not a surgery, but a complex medical procedure designed to replace a patient’s diseased bone marrow with healthy stem cells. In the context of leukemia, this serves two purposes:
- Replacement: It allows the patient to receive high doses of chemotherapy to kill cancer cells, knowing that the new stem cells will rebuild the immune system afterward.
- Immunotherapy: In allogeneic transplants (using a donor), the new immune system recognizes any remaining leukemia cells as foreign and attacks them—a powerful mechanism known as the Graft-Versus-Leukemia (GVL) effect.
The Procedure: Step by Step
The process is rigorous and requires a highly specialized medical environment:
- Conditioning: The patient receives high-dose chemotherapy and/or radiation. This clears the marrow of cancer cells and suppresses the immune system to prevent rejection of the new cells.
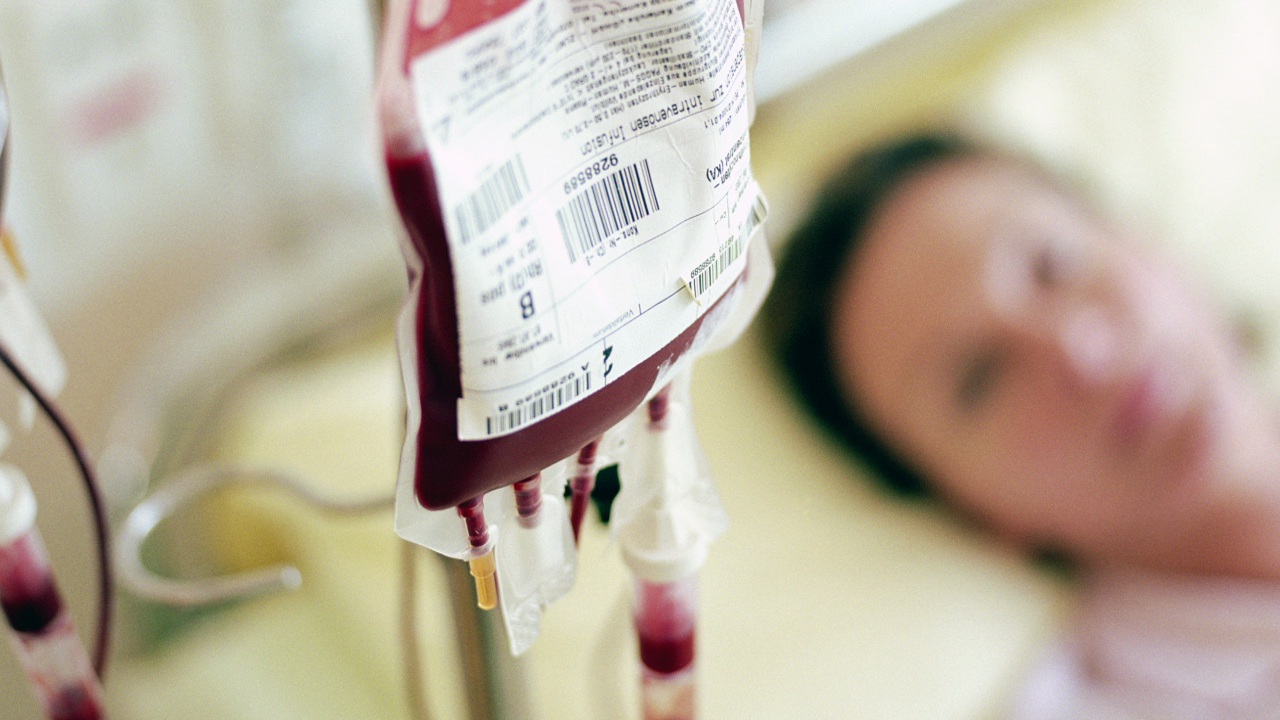
- Infusion: The healthy stem cells—harvested either from a donor (allogeneic) or sometimes the patient’s own stored cells (autologous)—are infused into the bloodstream through a catheter, similar to a blood transfusion.
- Engraftment: Over the next few weeks, these cells migrate to the bone marrow cavities and begin producing new, healthy blood cells.
Expert Care at Liv Hospital
The success of a stem cell transplant depends heavily on the expertise of the medical team and the quality of the post-procedure care. At Liv Hospital, our Hematology and Bone Marrow Transplantation Center adheres to international standards of safety and hygiene. We utilize HEPA-filtered isolation rooms to protect patients during the vulnerable engraftment phase and employ a multidisciplinary team to manage the complex immunological aspects of the transplant, ensuring the best possible chances for a successful recovery.